Humans are constantly surrounded by pathogens— disease-causing organisms such as bacterium, virus, parasite, or fungus— whether in the environment or within our bodies. Susceptible individuals who encounter harmful pathogens are at risk of developing life-threating diseases. Fortunately, the body is readily equipped with an immune system— a system capable of developing a series of protective defenses against pathogens as a natural response.
Immune System Mechanisms
There are two main parts to the immune system, namely the innate and adaptive immune system (Johns Hopkins Medicine, 2022). The innate immune system is an inborn rapid response system that includes physical barriers such as the skin, cornea, and mucous membrane lining in the respiratory, gastrointestinal, and genitourinary tract. The epidermis is composed of many layers of closely packed keratinized cells to prevent pathogens from entering the body in the first place. Mucous membrane secretes mucus, a sticky fluid that traps invading pathogens and dust. The protective physical barrier formed by mucus prevents pathogens from reaching the surface of the epithelium Other barriers such as tears, saliva, and urine contain lysozyme, a lytic enzyme that also functions as a cationic protein. Lysozyme kills bacteria by lysing bacterial cell well, peptidoglycan, to disrupt bacterial membrane and then activate autolytic enzymes in the bacterial cell for destruction (Ganz, 2006). Exposure to harmful germs, parasites, and cells do not result in immediate sickness because of these physical barriers. Should the pathogen infect the body, however, the system will recognize, then employ phagocytes such as neutrophils and macrophages to surround, cover, kill, and neutralize the invader immediately. Phagocytes find invading pathogens by causing inflammation, a sign of tissue injury cause by external trauma or infection. Upon tissue injury, mast cells will give out signaling molecules such as histamine, causing nearby capillaries to dilate. Neutrophils and monocytes will then migrate to the infected area through the widened capillary to conduct phagocytosis and prepare for tissue healing. If cells still get infected, interferon will be secreted. Interferon is an antiviral factor that “interferes” with viral replication to prevent further spreading (Kopitar-Jerala, 2017). Pathogens may also directly activate complement, a system of plasma proteins that “complements” the process of inflammation and phagocytosis. Although the body can provide a series of rapid innate immune responses, infections are not always cleared. In such cases, the acquired immune system will continue the body’s response.
The acquired immune system (with help from the innate immune system) creates antigen-specific antibodies to protect the body from a specific invader (National Center for Immunization and Respiratory Diseases, 2021). Each pathogen is composed of a several subparts unique to its molecular structure. The subpart of a pathogen that helps the immune system form antibodies is called an antigen. Macrophages swallow up and digest pathogens but leaves behind and presents the antigen part for lymphocytes to recognize then attack. When an antigen is detected, B-immune system responds by stimulating B-lymphocytes to produce antibodies to attack leftover pieces of the pathogen. While the B-lymphocytes directly attack pathogens using antibodies, T-lymphocytes attack pathogen-infected body cells. The human body is comprised of over a thousand antibodies, but each antibody is programmed to recognize only one specific antigen. After creating antigen-specific antibodies as a primary response, the immune system also produces antibody-producing memory B and T cells. Memory cells remain alive even after the antibodies have defeated a specific pathogen. The immune system takes time (up to several days) to produce antigen-specific antibodies during the body’s first encounter against a pathogen, but memory cells can recognize and directly produce specific antibodies to defend against it. Thus, the immune system will be able to respond rapidly if the body is exposed to the same antigen more than once in the future. By working together collaboratively and effectively in producing antigen-specific antibodies, natural immunity against a specific disease is achieved. Check the video below to learn how the immune system works using visuals:
Vaccine-induced Immunity
Immunity to a specific disease is achieved through the presence of antigen-specific antibodies, but only lasts for a certain time period. Although a newborn baby may acquire passive immunity (given antibodies) from its mother through the placenta, only active immunity (produce antibodies) is long-lasting or even life-long. Active immunity can be further categorized into two types, namely natural and vaccine-induced. According to the Division of Viral Diseases at the National Center for Immunization and Respiratory Diseases (2022), immunizations train the immune system to create antibodies as a form of protection against harmful diseases through vaccination. Vaccines are harmless variants of a pathogen used to stimulate the immune system to defend the body against specific pathogens and thereby, prevent specific diseases. Instead of containing the antigen itself, vaccines contain the blueprint for producing antigens. For numerous viral diseases such as measles and polio, prevention by vaccination is the only medical method to prevent illness.
Different types of vaccines may be made from different materials, but all types help protect the body against life-threatening diseases by stimulating the production of antigen-specific antibodies. For instance, mRNA Covid-19 vaccines contain material from SARS-Cov-2 (Covid-19-causing virus), protein subunit Covid-19 vaccines include harmless proteins from SARS-Cov-2, while vector vaccines contain viral vectors of SARS-Cov-2. All three of these materials are different, but all prompt the immune system to build B-lymphocytes and T-lymphocytes to fight a specific pathogen (in this case, SARS-Cov-2) if the body ever gets infected in the future. Several vaccines require multiple doses, given months or years apart to allow the production of long-lived antibodies and development of memory cells. Vaccines safely enable individuals to achieve immunity against a certain disease without having to be infected beforehand due to programmed memory. Vaccinated individuals are provided partial protection from infection, and protection from severe symptoms even if infection does occur as the body has prior experience in “fighting the same opponent”.
However, not every individual can be vaccinated. Those with underlying health conditions that weaken their immune systems (e.g. cancer, HIV) or allergies to specific vaccine components are unable to receive certain vaccines. Fortunately, they can still be protected if they live amongst others who are vaccinated— in a community with herd immunity (World Health Organization, 2020). Should the majority of people living in a community be vaccinated, the pathogen will be unable to circulate easily. Therefore, eligible individuals are highly advised to vaccinate themselves against life-threatening viral diseases, to protect themselves and others.
Impact of Lifestyle Factors on Immunity
Based on previous research done by Marsland et al. (2002) and Madison et al. (2021), psychological stress is known to affect immune function and vaccine efficacy. Individuals (even young and healthy students) who experienced significant stress and anxiety for a short period of time before getting vaccinated took a longer time to develop antibodies against hepatitis B, influenza, and pneumonia (Madison et al., 2021; Migala, 2021). Stressed individuals also experienced more side effects (e.g. fatigue and low mood) and reduced duration of immunity following a vaccine. According to Madison et al. (2021), stress and mental health conditions may lead to neuroendocrine or inflammatory changes that negatively alter vaccine efficacy, thereby necessitating a more frequent booster vaccination. Moreover, stressed and/or depressed individuals are more likely to perform unhealthy lifestyle habits, including lack of sleep, improper nutrition, and irregular exercise— all of which are factors that negatively affect antibody response following immunization.
Spiegel (2002) previously reported that short-term sleep deprivation prior to vaccination negatively impacts antibody count and thereby, efficacy of vaccines by lowering antibody count. More specifically, restricted sleep (< 4 hours) resulted in a >50% decrease of antibody production in response to influenza immunization. Sleep helps activate cytokine (IL-12 and IFN-γ) expression to regulate anti-viral immune defence mechanisms (Irwin, 2019). Sleep may also boost the number of antigen-presenting cells and T-lymphocytes (CD4+) (Lange et al., 2019), improving immunological memory formation. Meanwhile, sleep deprivation (<6 hours) results in decreased lymphocyte proliferation and innate immune cell activity against tumour and virus-infected cells by reducing up to 72% of natural killer cell activity (Frel et al., 2020). In other words, sleep plays a significant role in decreasing vulnerability and susceptibility to viral infection.
Childs et al. (2019) also demonstrated that adequate and appropriate nutrition is required for optimal immune function. Proper nutrition allows immune cells to initiate effective responses against pathogens as well as resolve unnecessary responses to avoid any underlying chronic inflammation (e.g. redness, swelling, feeling of heat and pain). For instance, micronutrients vitamin A and zinc regulate cell division to boost proliferative responses within the immune system, while the amino acid arginine helps macrophages generate nitric oxide to kill tumor cells while exerting anti-inflammatory effects (Childs et al., 2019). While undernutrition impairs immune function due to specific unmaintained roles in the immune system, overnutrition negatively alters leukocyte (including lymphocytes) count and cell-mediated immune responses. Overnutrition leads to obesity, which then results in immunodeficiency. Obesity-associated lipid build-up increases leptin (pro-inflammatory) and decreases adiponectin (anti-inflammatory) production, inducing chronic inflammation as an immune response (Heredia et al., 2012). Furthermore, obesity may result in insulin and leptin resistance, adipose tissue expansion, as well as decreased pancreas β-cell function, all of which limit metabolic responses to immunity challenges through the development of comorbidities such as Type 2 diabetes, cardiovascular diseases, hypertension, and cancer (Hardy et al., 2012; Kasuga, 2006). According to Mohammad et al. (2021), these changes negatively impair immune cell growth and proliferation, host immune defense, and glucose metabolism. Expanded ACE-2 adipose tissue could also spread infectious diseases such as Covid-19 to other tissues, increasing severity of disease. Thus, chronic inflammation and metabolic dysfunction caused by both undernutrition and overnutrition dysregulate innate immune system mechanisms, resulting in an increased risk of infectious disease susceptibility, severity, and mortality.
Additionally, Silveira et al. (2021) suggests that regular moderate-intensity physical exercise (at least 150 minutes every week) strengthens the immune system by modulating cellular immunity. During and after physical exercise, pro- and anti-inflammatory cytokines are released, while lymphocyte recruitment and circulation is increased. Such changes are associated with the reduction of excessive weight, increased physical and cardiopulmonary conditioning, optimal pro-inflammatory and pro-thrombotic states, decreased oxidative stress, and improved glycemic, insulinic, and lipidic metabolisms. Similar to the impact of optimal nutrition, regular physical exercise prevents obesity, and positively impacts all the factors that would be negatively altered by obesity. Therefore, the practice of regular physical exercise may help lower the risk of viral infections, as well as the intensity of severe symptoms and incidence of mortality caused by infections.

Autoimmune Diseases (Naturally- and Vaccine Induced)
Although the immune system is responsible for defending the body against foreign pathogenic cells, the system may also mistakenly attack itself by targeting normal cells, thereby causing an autoimmune disease. There are around 80 autoimmune diseases of varying severity. Common autoimmune diseases include rheumatoid arthritis, lupus, coeliac disease, multiple sclerosis, type 1 diabetes, alopecia areata, and vasculitis.
According to Rosenblum et al. (2015), genetic susceptibility, environmental stimuli, and defective regulation are the main factors responsible for initiating autoimmunity. Genetic polymorphisms in immune-related genes such as HLA may result in a reduced threshold for autoreactive T-lymphocyte activation. T-cells are activated when enough T-cell receptors (TCR) are triggered by a presented antigen. Based on previous research conducted by Viola & Lanzavecchia (1996), the normal activation threshold is 8000 TCRs, but reduced thresholds require only 1500 TCRs for T-cells to respond to antigenic stimulation. On the other hand, environmental factors such as infection, the microbiome, or traumatic insult that create a pro-inflammatory environment initiates the activation of autoreactive T-lymphocytes. Regulatory T-cells (Tregs) are employed to suppress autoreactive T-cells to avoid unnecessary immune responses through the inhibition of T-cell proliferation (Kondelkova et al., 2010). However, defects in development, stability, or function may render Tregs dysfunctional, thereby unable to control autoreactive T-cell activity. Autoreactivity refers to immune responses against self-constituents such as healthy cells and issues, which then results in autoimmunity.
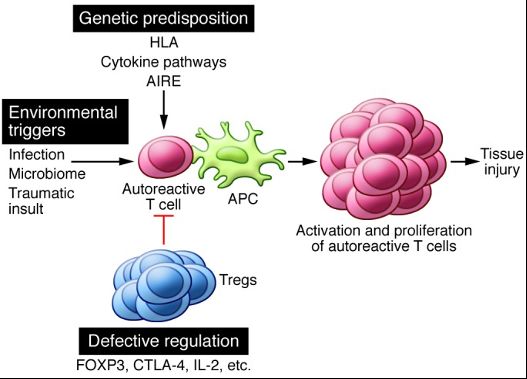
An example of an autoimmune disease caused by environmental stimuli is psoriatic arthritis. Psoriasis is a skin condition characterized by scales and itchy, dry patches. Environmental triggers for psoriasis include infections, cold, and psychological stress. An autoimmune reaction that affects the joints of psoriasis patients may then develop as a response to injury or high physical stress. For instance, a runner often experiences heel tendon damage as the muscle is constantly pulling on the bone to create movement. Repeated and long-term stress to the tendon exposes tissue that should not be in contact with blood cells. Once exposed, the immune system deploys blood cells to treat the exposure like a wound, but an abnormal immune response could cause inflammation of the joints and tendons (Orbai, 2022).
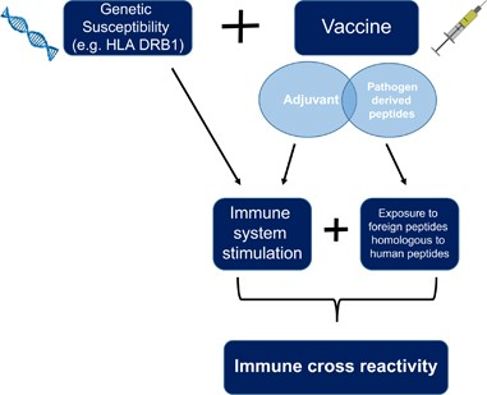
A topic of unending debate in medical literature is whether vaccines (e.g. influenza, hepatitis b, and human papilloma virus vaccine) may lead to allergies and autoimmune diseases (e.g. multiple sclerosis, rheumatoid arthritis, and vasculitis) via molecular mimicry— a significant similarity between certain vaccine-contained pathogenic elements and specific human proteins. Segal & Shoenfeld (2018) state that this similarity may result in immune cross-reactivity. Based on previous research, the human proteome shares up to 90% of viral pentapeptides and 99.7% of bacterial heptapeptides (Kanduc, 2010; Kanduc et al., 2008), indicating a high probability of immune cross-reactivity.
However, Kanduc (2012) demonstrated that the immune system may perform tolerogenic mechanisms (Treg activation and proliferation as a second signal) to prevent autoimmunity. It was then suggested that an environmental factor— adjuvants— a variety of compounds added in a vaccine to stimulate immune response— impairs immune tolerance. Another counterargument, however, would be that immune responses to shared pathogenic elements is only possible due to the addition of adjuvants. Thus, the same genetic factor that causes autoimmunity— HLA DRB1— was suggested as another significant environmental trigger. In conclusion, exposure to shared pathogenic motifs and impaired immune tolerance as a result of genetic susceptibility and presence of adjuvants may result in autoimmunity after immunization.
Proper Behavioral Response to Vaccines
In receiving vaccines, individuals are encouraged to maintain a cheerful, relaxed, and energetic mood. Based on a study done by Marsland et al. (2006), individuals with an overall happy and positive mood produced a 73% greater antibody response to hepatitis B vaccines as compared to those who reported feeling nervous, tense, or angry. According to Zaraska (2021), psychological and behavioral factors may significantly affect vaccine efficacy, specifically antibody production and inflammatory response. Optimism is known to switch immune-related genes away from an inflammatory response when preparing to defend the body from pathogens (Zaraska, 2021). Thus, individuals are highly recommended to get vaccinated with a positive state of mind. Cedars Sinai Hospital (2021) suggests 5 mood-lifting tips, namely to de-stress, sleep enough, connect socially, exercise, and cultivate gratitude to help boost your immunity after vaccinations.
Experience & Conclusion
Based on the explanation above, there is no need to worry about developing autoimmune diseases as a result of vaccines unless you are already aware of very rare personal genetic predispositions. Instead, the CDC recommends all individuals to receive vaccines for chickenpox, dengue, diphtheria, influenza, hepatitis A, hepatitis B, Hib (Haemophilus influenzae type b), HPV (human papillomarvirus), measles, meningococcal, mumps, pneumococcal, polio, rotavirus, rubella, shingles, tetanus, and whooping cough to prevent the infection of life-threatening diseases. The Indonesian Ministry of Health specifically made 5 types of vaccines, namely hepatitis B, tuberculosis (BCG), polio, a combination of diphtheria, pertussis, and tetanus (DPT-HB), and measles mandatory for all Indonesian babies. As someone who has received all 5 vaccines as a baby and never contracted any of the infections the vaccine was made to prevent even 17 years later, I can testify that getting vaccinated according to the recommendation given by both global and national health agencies is a beneficial and laudable choice. The WHO also strongly urges all individuals to get vaccinated against the highly infectious SARS-CoV-2 using whatever Covid-19 vaccine brand is available during this pandemic. As someone whose whole family has received the full Covid-19 vaccine dosage and never been infected with Covid-19 despite thousands of new national cases each day, I myself would also advise you to get vaccinated against Covid-19 immediately. Should you still be worried of developing allergies, you can choose to stay in the immunization venue for at least 30 minutes to consult with a present doctor.
Remember that it is important to maintain a cheerful and positive mindset for optimum antibody response when receiving vaccines. Lastly, proper sleep (>6 hours every night), adequate nutrition, and regular exercise should be enacted in your daily life to boost overall health and immunity. These factors should not only be considered for a week before getting vaccinated or during Covid-19 waves, but as a lifestyle as it benefits your own health and well-being. Protecting yourself should be a priority, and by doing so, you are also protecting your loved ones and the others around you. So, #AyoVakinCovid-19! Click here to register for a Covid-19 vaccine in Indonesia.
References
- Childs, Calder, & Miles. (2019). Diet and Immune Function. Nutrients, 11(8), 1933. https://doi.org/10.3390/nu11081933
- Silveira, M. P., da Silva Fagundes, K. K., Bizuti, M. R., Starck, É., Rossi, R. C., & de Resende e Silva, D. T. (2021). Physical exercise as a tool to help the immune system against COVID-19: an integrative review of the current literature. Clinical and Experimental Medicine, 21(1), 15–28. https://doi.org/10.1007/s10238-020-00650-3
- Frel, D. L., Atsma, D. E., Pijl, H., Seidell, J. C., Leenen, P. J. M., Dik, W. A., & van Rossum, E. F. C. (2020). The Impact of Obesity and Lifestyle on the Immune System and Susceptibility to Infections Such as COVID-19. Frontiers in Nutrition, 7. https://doi.org/10.3389/fnut.2020.597600
- Heredia, F. P., Gómez-Martínez, S., & Marcos, A. (2012). Obesity, inflammation and the immune system. Proceedings of the Nutrition Society, 71(2), 332–338. https://doi.org/10.1017/S0029665112000092
- Ganz, T. (2006). LYSOZYME. In Encyclopedia of Respiratory Medicine (pp. 649–653). Elsevier. https://doi.org/10.1016/B0-12-370879-6/00228-3
- Hardy, O. T., Czech, M. P., & Corvera, S. (2012). What causes the insulin resistance underlying obesity? Current Opinion in Endocrinology, Diabetes & Obesity, 19(2), 81–87. https://doi.org/10.1097/MED.0b013e3283514e13
- Irwin, M. R. (2019). Sleep and inflammation: partners in sickness and in health. Nature Reviews Immunology, 19(11), 702–715. https://doi.org/10.1038/s41577-019-0190-z
- Johns Hopkins Medicine. (2022). The Immune System. Johns Hopkins Medicine.
- Kanduc, D. (2010). The self/nonself issue: A confrontation between proteomes. Self/Nonself, 1(3), 255–258. https://doi.org/10.4161/self.1.3.11897
- Kanduc, D. (2012). Peptide cross-reactivity the original sin of vaccines. Frontiers in Bioscience, S4(4), 341. https://doi.org/10.2741/s341
- Kanduc, D., Stufano, A., Lucchese, G., & Kusalik, A. (2008). Massive peptide sharing between viral and human proteomes. Peptides, 29(10), 1755–1766. https://doi.org/10.1016/j.peptides.2008.05.022
- Kasuga, M. (2006). Insulin resistance and pancreatic cell failure. Journal of Clinical Investigation, 116(7), 1756–1760. https://doi.org/10.1172/JCI29189
- Kopitar-Jerala, N. (2017). The Role of Interferons in Inflammation and Inflammasome Activation. Frontiers in Immunology, 8. https://doi.org/10.3389/fimmu.2017.00873
- Lange, T., Born, J., & Westermann, J. (2019). Sleep Matters: CD4+ T Cell Memory Formation and the Central Nervous System. Trends in Immunology, 40(8), 674–686. https://doi.org/10.1016/j.it.2019.06.003
- Madison, A. A., Shrout, M. R., Renna, M. E., & Kiecolt-Glaser, J. K. (2021). Psychological and Behavioral Predictors of Vaccine Efficacy: Considerations for COVID-19. Perspectives on Psychological Science, 16(2), 191–203. https://doi.org/10.1177/1745691621989243
- Marsland, A., Bachen, E., Cohen, S., Rabin, B., & Manuck, S. (2002). Stress, immune reactivity and susceptibility to infectious disease. Physiology & Behavior, 77(4–5), 711–716. https://doi.org/10.1016/S0031-9384(02)00923-X
- Marsland, A. L., Cohen, S., Rabin, B. S., & Manuck, S. B. (2006). Trait positive affect and antibody response to hepatitis B vaccination. Brain, Behavior, and Immunity, 20(3), 261–269. https://doi.org/10.1016/j.bbi.2005.08.009
- Migala, J. (2021). Can Diet and Lifestyle Choices Affect COVID-19 Vaccine Efficacy? Everyday Health.
- Mohammad, S., Aziz, R., al Mahri, S., Malik, S. S., Haji, E., Khan, A. H., Khatlani, T. S., & Bouchama, A. (2021). Obesity and COVID-19: what makes obese host so vulnerable? Immunity & Ageing, 18(1), 1. https://doi.org/10.1186/s12979-020-00212-x
- National Center for Immunization and Respiratory Diseases. (2021). Antibodies and COVID-19. Centers for Disease Control and Prevention.
- National Center for Immunization and Respiratory Diseases. (2022). Understanding How COVID-19 Vaccines Work. Centers for Disease Control and Prevention.
- Orbai, A.-M. (2022). Autoimmune Disease: Why Is My Immune System Attacking Itself? Johns Hopkins Medicine.
- Rosenblum, M. D., Remedios, K. A., & Abbas, A. K. (2015). Mechanisms of human autoimmunity. Journal of Clinical Investigation, 125(6), 2228–2233. https://doi.org/10.1172/JCI78088
- Segal, Y., & Shoenfeld, Y. (2018). Vaccine-induced autoimmunity: the role of molecular mimicry and immune crossreaction. Cellular & Molecular Immunology, 15(6), 586–594. https://doi.org/10.1038/cmi.2017.151
- Spiegel, K. (2002). Effect of Sleep Deprivation on Response to Immunizaton. JAMA, 288(12), 1471. https://doi.org/10.1001/jama.288.12.1469
- Viola, A., & Lanzavecchia, A. (1996). T Cell Activation Determined by T Cell Receptor Number and Tunable Thresholds. Science, 273(5271), 104–106. https://doi.org/10.1126/science.273.5271.104
- World Health Organization. (2020). How do vaccines work?
- Zaraska, M. (2021). Positive mood and good friends can boost response to vaccines. New Scientist, 249(3317), 11. https://doi.org/10.1016/S0262-4079(21)00036-1
Follow Instagram @kompasianacom juga Tiktok @kompasiana biar nggak ketinggalan event seru komunitas dan tips dapat cuan dari Kompasiana. Baca juga cerita inspiratif langsung dari smartphone kamu dengan bergabung di WhatsApp Channel Kompasiana di SINI











